|
Overview, Anatomy and Embryology, Primary Hyperparathyroidism. Definition of problem. 
Primary hyperparathyroidism is the unregulated overproduction of parathyroid hormone (PTH) resulting in abnormal calcium homeostasis. Frequency. US population- based data from Olmsted County, Minn, indicate that the prevalence of primary hyperparathyroidism is slowly decreasing. The mean age at diagnosis has remained between 5. Etiology. In approximately 8. In 1. 5% of cases, multiple glands are involved (ie, either multiple adenomas or hyperplasia). The etiology of adenomas or hyperplasia remains unknown in most cases. Familial cases can occur either as part of the multiple endocrine neoplasia syndromes (MEN 1 or MEN 2a), hyperparathyroid- jaw tumor (HPT- JT) syndrome, or familial isolated hyperparathyroidism (FIHPT). Familial hypocalciuric hypercalcemia and neonatal severe hyperparathyroidism also belong to this category. The molecular genetic basis of MEN 1 is an inactivating mutation of the MEN1 gene, located on chromosome band 1. MEN 2a is caused by a germline mutation of the Ret proto- oncogene on chromosome 1. However, this is not the case in primary hyperparathyroidism from parathyroid hyperplasia. An increase in the cell numbers is probably the cause. The chronic excessive resorption of calcium from bone caused by excessive parathyroid hormone can result in osteopenia. In severe cases, this may result in osteitis fibrosa cystica, which is characterized by subperiosteal resorption of the distal phalanges, tapering of the distal clavicles, salt- and- pepper appearance of the skull, and brown tumors of the long bones. This is not commonly seen now.  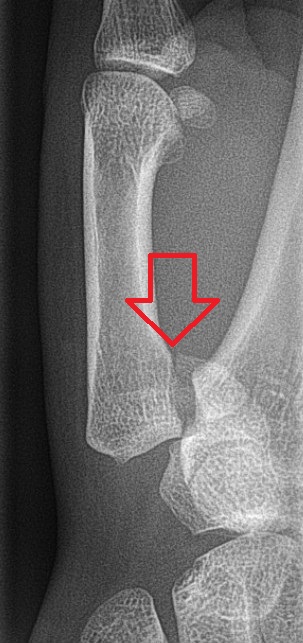    
Gpnotebook Osteoporosis Diet YoutubeDiabetes Mellitus is the Latin name for diabetes. Type 1 diabetes mellitus occurs when the body cannot produce sufficient insulin to absorb blood sugar. In addition, the chronically increased excretion of calcium in the urine can predispose to the formation of renal stones. The other symptoms of hyperparathyroidism are due to the hypercalcemia itself and are not specific to hyperparathyroidism. These can include muscle weakness, fatigue, volume depletion, nausea and vomiting, and in severe cases, coma and death. Neuropsychiatric manifestations are particularly common and may include depression, confusion, or subtle deficits that are often characterized poorly and may not be noted by the patient. Increased calcium can increase gastric acid secretion, and persons with hyperparathyroidism may have a higher prevalence of peptic ulcer disease. Rare cases of pancreatitis have also been attributed to hypercalcemia. Clinical presentation. History. The clinical syndrome of primary hyperparathyroidism can be easily remembered as . Bone and joint pain, pseudogout, and chondrocalcinosis have also been reported. In the early clinical description of primary hyperparathyroidism, some patients developed a peculiar type of bone disease known as osteitis fibrosa cystica, characterized by increased generalized osteoclastic bone resorption, particularly involving the phalanges causing subperiosteal resorption, and the skull causing the radiologic appearance known as salt and pepper skull. This presentation is rarely seen today except in medically underserved populations. Renal manifestations include polyuria, kidney stones, hypercalciuria, and rarely nephrocalcinosis. Gastrointestinal manifestations include anorexia, nausea, vomiting, abdominal pain, constipation, peptic ulcer disease, and acute pancreatitis. Neuromuscular and psychologic manifestations include proximal myopathy, weakness and easy fatigability, depression, inability to concentrate, and memory problems or subtle deficits that are often characterized poorly and may not be noted by the patient. Cardiovascular manifestations include hypertension, bradycardia, shortened QT interval, and left ventricular hypertrophy. Examination may reveal muscle weakness and depression. A palpable neck mass is not usually expected with hyperparathyroidism, although in rare cases, it may indicate parathyroid cancer. Diagnostic considerations. The causes of hypercalcemia that result in a concomitantly elevated parathyroid hormone level are few. These include familial benign (hypocalciuric) hypercalcemia (FHH) (see Related disorders), lithium- induced hypercalcemia, and tertiary hyperparathyroidism. A minority of patients (ie, 1. A subset of patients have calcium levels within the reference range with elevated parathyroid hormone, so- called normocalcemic hyperparathyroidism. However, when considering this diagnosis, all potential causes of secondary hyperparathyroidism (eg, low calcium intake, gastrointestinal disorders, renal insufficiency, vitamin D deficiency, hypercalciuria of renal origin) should be excluded. Patients with normal calcium levels and elevated parathyroid hormone levels in the absence of an identifiable secondary cause should be monitored for progression to hypercalcemia. Secondary and tertiary hyperparathyroidism are typically diagnosed based on their clinical context. Cancer- induced hypercalcemia is usually associated with a low parathyroid hormone level but possibly a high parathyroid hormone- related peptide level. Workup. Laboratory studies. Total serum calcium and albumin levels or ionized calcium levels should be measured. Hypercalcemia should be documented on more than one occasion before a diagnostic workup is undertaken. Testing of the intact parathyroid hormone level is the core of the diagnosis. An elevated intact parathyroid hormone level with an elevated ionized serum calcium level is diagnostic of primary hyperparathyroidism. A 2. 4- hour urine calcium measurement is necessary to rule out FHH. Older assays measured fragments of the parathyroid hormone molecule, such as the C- terminal or mid region of parathyroid hormone. These first- generation assays are considered obsolete for the clinical practice. Second- generation parathyroid hormone assays, globally called . Second- and third- generation parathyroid hormone assays are producing far more clinically satisfying data than the first- generation assays but have some limitations that continue to be assessed in several studies. Other laboratory findings in primary hyperparathyroidism include mild hyperchloremic acidosis, hypophosphatemia, and mild- to- moderate increase in urinary calcium excretion rate. A study by Saliba et al evaluated the relationship between 2. OH)D levels and concomitant parathyroid hormone levels. The results revelaed that a 2. OH)D threshold of 5. L is sufficient for parathyroid hormone suppression and prevention of secondary hyperparathyroidism in persons with normal renal function. Gpnotebook Osteoporosis Diet TherapyOH)D levels that are greater than 7. L were not associated with additional changes in parathyroid hormone levels. Imaging studies are used to guide the surgeon once surgical therapy has been decided. If a limited parathyroid exploration is to be attempted, a localizing study is necessary. Other uses of imaging studies in the initial evaluation of a patient with primary hyperparathyroidism are controversial (see Choice of surgical treatment, below). For many patients, the recommendation remains for complete parathyroid exploration with resection of all involved glands. Many surgeons agree that imaging studies are not required when this surgical treatment is chosen. However, in patients who have recurrent or persistent hyperparathyroidism after a previous surgical exploration, an imaging test to localize involved glands is definitely indicated. Ultrasonography of the neck is a safe and widely used technique for localization of abnormal parathyroid glands. It is capable of a high degree of accuracy, but it is operatordependent and its reported accuracy has varied widely in the literature. Find medical information for Pizotifen including its uses, side effects and safety, interactions, pictures, and warnings. Low back pain; Synonyms: Lower back pain, lumbago: Low back pain is a common and costly complaint. Pronunciation. This page includes the following topics and synonyms: Hyperparathyroidism, Primary Hyperparathyroidism. Guide to type 2 diabetes symptoms and how long type 2 diabetes symptoms may take to develop. Type 2 diabetes symptoms include frequent urination, constant thirst. 
One advantage of neck ultrasonography is that it can be performed rapidly by the clinician at the time of the initial evaluation. Studies of clinician- performed ultrasound show accuracy rates that compare favorably with the accuracy of traditional radiology departments, in the vicinity of 7. Continued How are Bartholin gland cysts diagnosed? You may find a Bartholin gland cyst on your own, or your doctor may notice it during a physical exam. Sestamibi is commonly used in cardiac imaging and was found serendipitously to accumulate in parathyroid adenomas. This radionuclide is concentrated in thyroid and parathyroid tissue but usually washes out of normal thyroid tissue in under an hour. It persists in abnormal parathyroid tissue. See the image below. On delayed images, an abnormal parathyroid is seen as a persistent focus of activity. The scan's sensitivity for detecting solitary adenomas has varied widely in the literature but generally is reported as 6. The main weakness of this test is in diagnosing multiglandular disease. In this case, sensitivity drops to approximately 5. The scan can include the mediastinum and, thus, is extremely useful in cases of an ectopic adenoma or previously failed surgical exploration. CT scanning and magnetic resonance imaging (MRI) have also been used also to locate abnormal parathyroid glands. Standard CT scanning has inadequate sensitivity. Newer techniques of CT scanning with dynamic contrast images (4. D- CT) have shown promise, with accuracy rates as high as 8. Note that hyperparathyroidism preferentially affects the cortical bone at the radius (distal third). In cases of severe primary hyperparathyroidism, skeletal radiographs show pathognomonic changes such as salt- and- pepper degranulation in the skull and subperiosteal bone resorption in the phalanges. Procedures. Bilateral internal jugular vein sampling is used to help localize ectopic parathyroid adenomas; however, this technique should generally be reserved for centers with specialists and for selected patients. Treatment. Surgical excision of the abnormal parathyroid glands (see below for details of surgical treatment) offers the only permanent, curative treatment for primary hyperparathyroidism. There is universal agreement that surgical treatment should be offered to all patients with symptomatic disease. Some controversy exists regarding the optimal management of asymptomatic patients. A National Institutes of Health (NIH) Workshop on Asymptomatic Primary Hyperparathyroidism in 2. NIH Consensus Development Conference. The indications for surgery as per the 2. Bartholin Gland Cyst Symptoms, Causes, Treatments. What are the Bartholin glands? The Bartholin glands are two small organs under the skin in a woman's genital area. They are on either side of the folds of skin (labia) that surround the vagina and urethra. Most of the time, you can't feel or see these glands. The Bartholin glands make a small amount of fluid that moistens the outer genital area, or vulva. This fluid comes out of two tiny tubes next to the opening of the vagina. These tubes are called Bartholin ducts. What are Bartholin gland cysts? If a Bartholin duct gets blocked, fluid builds up in the gland. The blocked gland is called a Bartholin gland cyst. They usually grow slowly. If the Bartholin gland or duct gets infected, it's called a Bartholin gland abscess. Bartholin gland cysts are often small and painless. Some go away without treatment. But if you have symptoms, you might want treatment. If the cyst is infected, you will need treatment. What causes a Bartholin gland cyst? Things like an infection, thick mucus, or swelling can block a Bartholin gland duct and cause a cyst. The cyst can get bigger after sex, because the glands make more fluid during sex. Infected Bartholin cysts are sometimes caused by sexually transmitted infections (STIs). You can lower your risk of STIs by using a condom when you have sex. What are the symptoms? You may not have any symptoms if the Bartholin gland cyst is small. But a large cyst or an infected cyst (abscess) can cause symptoms. Symptoms of a cyst that is not infected include: A painless lump in the vulva area. Redness or swelling in the vulva area. Discomfort when you walk, sit, or have sex. Symptoms of an infected cyst include: Pain that gets worse and makes it hard to walk, sit, or move around. Fever and chills. Swelling in the vulva area. Drainage from the cyst. Continued. How are Bartholin gland cysts diagnosed? You may find a Bartholin gland cyst on your own, or your doctor may notice it during a physical exam. Unless it is causing symptoms, you may not know you have one. An abscess is diagnosed based on signs of infection, such as fever or swelling, and pain in the vulva area. In some cases, especially if you are older, your doctor may remove the cyst to make sure that it isn't cancer or another problem. How are they treated? Some Bartholin gland cysts go away without treatment. You can take a nonprescription pain medicine such as ibuprofen (Advil or Motrin, for example) to relieve pain. To help healing, soak the area in a shallow, warm bath, or a sitz bath. Don't have sex while a Bartholin cyst is healing. If the cyst is infected, it may break open and start to heal on its own after 3 to 4 days. But if the cyst is painful, your doctor may drain it. You may also need to take antibiotics to treat the infection. To keep the cyst from closing and filling up again, your doctor may put a small drainage tube with a small balloon at one end inside the cyst. The balloon is inflated inside the cyst to keep the cyst open. After the gland has healed, the tube and balloon are removed. Sometimes a carbon dioxide laser or silver nitrate is used to prevent a cyst from growing back. For severe cysts that keep coming back, you may have surgery to remove the Bartholin gland and duct. There is a procedure called marsupialization in which a pouch is created by making a cut over the cyst and stitching the sides together. This allows the cyst to drain. Web. MD Medical Reference from Healthwise. This information is not intended to replace the advice of a doctor. Healthwise, Healthwise for every health decision, and the Healthwise logo are trademarks of Healthwise, Incorporated.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
November 2017
Categories |
 RSS Feed
RSS Feed
